Whether surfing the internet, looking at Instagram or watching television, everywhere you look there is talk about COVID-19. A lot of the conversation about COVID-19 centers on the medical devices used for testing. From early on in the pandemic, medical device manufacturers have focused on better tests, better testing methods and ways to get faster results. But how do these tests measure up in terms of use, device safety and reliability?
The Medical Devices Behind COVID-19 Tests
As the pandemic continues, many manufacturers are offering promising testing methods that could help the healthcare system identify COVID-19 patients quicker and with more effectiveness. Below is more information about current testing methods and the promising medical devices that could change the way doctors detect COVID-19.
PCR Tests
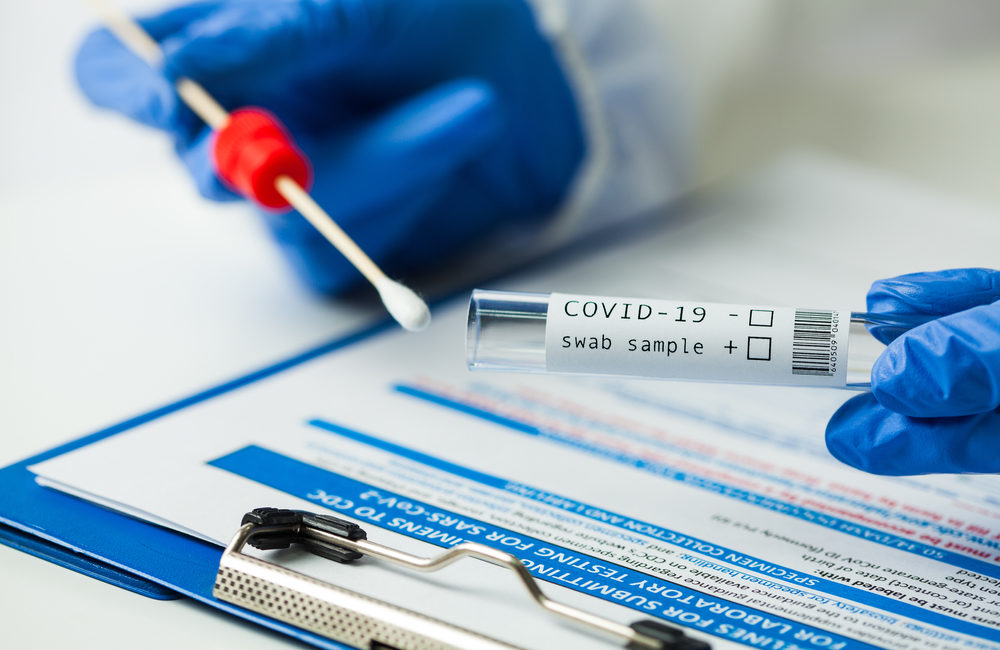
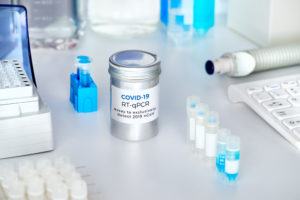
For most of the pandemic, polymerase chain reaction (PCR) and antibody tests have been the standard. These methods are still in use on a global scale. PCR tests work by detecting genetic information about the virus, or the RNA. The success of an accurate PCR test relies on the patient having an active infection.
PCR tests also work by detecting the presence of viral antigens, rather than looking for antibodies, or the body’s response to the virus. Viral RNA is present in the body before antibodies are developed, and often, before the patient has symptoms. This is important in helping doctors detect the virus early.
According to Dr. Edward Wright, a senior lecturer in microbiology,
“PCR gives us a good indication of who is infected. They can be isolated and get in contact with people they’ve been in touch with so they can be quarantined too, just in case. That’s the true advantage of the current major diagnostic tests, you can break that transmission chain and get a clearer picture of what’s happening.”
While PCR is a great testing method for early detection, the method is not without flaws. Processing PCR tests is very labor intensive. Also, there are several stages in the process, which leaves more room for errors. Errors can lead to false negatives, which occur in around 30 percent of PCR tests.
Scientists note that since the start of the COVID-19 pandemic, PCR testing methods have been refined. Greater automation and better medical devices have resulted in an 80-85 percent chance that the test will accurately detect the virus.
Serologic Tests
Serologic tests don’t tell doctors who is infected, but it can help in determining what percent of the population has been infected. Antibodies are generated by the body a week or two after the virus starts. This is generally around the time that the virus begins to clear. Serologic tests use blood samples instead of fluid samples, which is where antibodies are detected.
Serologic testing is helpful because it allows public health officials to determine, theoretically, what proportion of the population has immunity to the virus. If enough people develop immunity, then the virus won’t circulate through the population like it currently is. This is what is known as “herd immunity.”
Lateral Flow Assay Tests
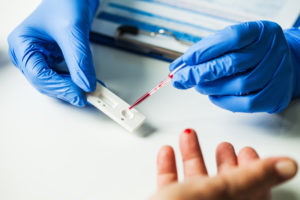
One of the medical devices being developed as a possible quick-response testing method is the lateral flow assay test. Canadian company Sona Nanotech is working on a rapid screening test for COVID-19. Lateral assay tests are inexpensive and easy to use, which makes them a great option for the general public. These tests also use a variety of samples, including blood, urine, saliva and other fluids.
One of the most common examples of a lateral flow assay test is pregnancy tests. These tests look for a specific biological marker in the test. For COVID-19, these tests could accurate identify the biological markers of the virus, with results produced in five to 15 minutes.
Sona Nanotech owns a proprietary gold nanorod technology. This can be used in numerous lateral flow assay applications. The nanorod binds to certain biological materials and carries them down a test strip. This is how the test produces a positive or negative result. Sona is working to develop a test that will specifically detect COVID-19.
Rapid Antigen Testing
Bosch is another company working on developing a COVID-19 test that produces faster results. The company is developing a point of care swab test that will present results in less than two and a half hours. Bosch is using their pre-existing Vivalytic analysis device to design the new COVID-19 test. They say it is one of “the world’s first fully automated molecular diagnostic tests” that could be directly used by all medical facilities.
The Vivalytic test uses two cartridges that each contain biological components. The cartridges detect SARS-CoV-2, or COVID-19, and can detect nine other respiratory viruses. This would be useful if the patient has respiratory symptoms, but tested negative for COVID-19. The Vivalytic test could then help healthcare providers determine the best course of treatment.
Could Medical Devices Stop the Spread of COVID-19?
There is no single medical device that can stop the spread of COVID-19. However, antigen tests like those being developed by Sona and Bosch can better identify active infections. Antigen tests do not require laboratory processing and, therefore, are less expensive and produce results faster. Dr. Wright says,
“The more testing you do the clearer the picture is on who is infected and thus who needs to be isolated.”
It is noted that countries like South Korea and Germany have a higher testing capability than many others. These countries have experienced a much smoother progression of the pandemic. With better testing comes better results, and that is the key to helping communities stop the spread of COVID-19.
Sources: