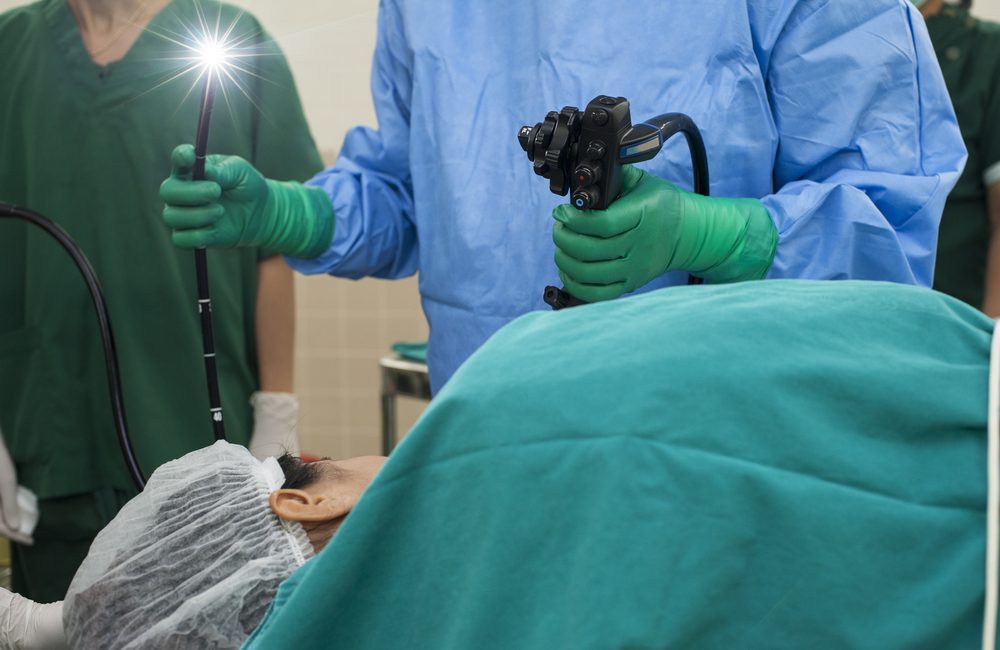
After years of improvement in the rate of medical scope infections, the U.S. Food and Drug Administration (FDA) recently began receiving reports of superbug infections associated with contaminated medical scopes.
In 2015, the high rate of infections prompted the FDA to require medical scope manufacturers to conduct post-market studies on the rates of infection related to their products. Infection rates were on the decline until March 2019, when preliminary results indicated “higher than expected levels of contamination.”
Medical Scope Infections
The FDA made headlines in April 2019, providing an update with more disturbing information about medical scope-related infections. The update was an announcement that, in light of high rates of infection, the agency is continuing the process it began in 2015 to collect samples and information about the infections.
In October 2015, the FDA ordered all three manufacturers of duodenoscopes – Fujifilm Medical Systems USA, Inc, Olympus Medical Systems Corporation, and Pentax of America – to begin post-market studies about their product. This requirement came after the FDA received 250 reports of patients who contracted a medical scope infection that year.
Despite convening panels of experts to advise new procedures and issuing strict orders to manufacturers to adhere to the procedures and report back, the FDA reports the number of medical scope infections doubled from 2017 to 2018. Even though hospital staff members are using the stringent cleaning and processing methods the FDA requires, patients are still getting sick. Some contract infection from antibiotic-resistant superbugs and die from the illness.
Superbug Infections Associated with Medical Scopes
The FDA has reported that medical scopes are contributing to more than just infections. They are causing deadly outbreaks of a superbug known as carbapenem-resistant Enterobacteriaceae (CRE). CRE is the multi-drug resistant bacteria associated with the medical scope infections currently under scrutiny. CRE outbreaks are a public health concern because there are not many treatment options for this superbug.
Strains of bacteria that are resistant to most common antibiotics are called superbugs and can cause:
- Pneumonia
- Urinary tract infections (UTI)
- Skin infections
Like other harmful bacteria such as E. coli, CRE can be present in the digestive tract without causing any problems. Infection happens when the bacteria spreads to the bloodstream or to other parts of the body.
Contracting the infection is desperately serious. Mortality rates for patients with CRE are 40-50 percent. Medical scope procedures provide the perfect avenue for serious CRE infections to spread to patients who later receive an ERCP with the same scope. Worse, ERCP patients are usually already ill and unable to fight drug-resistant bacteria.
How Patients Contract Infections from Contaminated Medical Scopes
The medical scopes in question are used in Endoscopic Retrograde Cholangiopancreatography procedures (ERCP). These devices are complex, delicate, and expensive instruments that have many small moving parts where bacteria can remain after use. Detailed processing is necessary between patients before reusing these $30,000 instruments.
The prevailing theory is that inattentive and ineffective cleaning methods have allowed tissue or fluid containing bacteria to remain behind on the scope and pass infection on to the next patient. The FDA’s recent statement indicated that meticulous disinfection and processing reduces the risk of medical scope infection, but does not eliminate it.
What is an ERCP?
An ERCP is an exploratory procedure involving a duodenoscope – a small camera at the end of a long, thin tube. A doctor passes the scope through the mouth, down the esophagus, and into the top of the small intestine, called the duodenum. The camera allows a doctor to examine the tubes and vessels that drain the liver, gallbladder, and pancreas and provides diagnostic information that doctors can’t obtain through an X-ray, ultrasound, CT scan, or MRI.
An ERCP may be used to:
- Take tissue samples
- Check for the cause of persistent abdominal pain or jaundice
- Remove or pulverize gallstones
- Open blocked entry ducts to the bowel
- Drain blocked areas
- Repair strictures (narrow passages)
For patients who need an ERCP, the procedure can be life-saving. That is why the FDA has taken regulatory steps in lieu of asking for a recall. At this point, the data seems to indicate more people are helped than are harmed by medical scopes. The risk of infection does not outweigh the benefit a very sick patient will receive from a successful ERCP.
How Common are CRE infections from ERCP?
ERCP is a common procedure, especially among gastrointestinal patients. Here are some statistics about the procedure and related infections:
- Surgeons perform up to 600,000 ERCPs each year
- 215 patients suffered infection following ERCP in 2015
- Fewer than 100 patients reported infection in 2016
- 205 patients submitted medical device reports about medical scopes between October 15, 2018 and March 31, 2019, of these:
- 159 were reports of medical scope contamination
- 1 report was of a patient exposed to contamination
- 45 reports were of medical scope infection
- 3 deaths from medical scope infection were reported to the FDA in 2018
CRE infection remains somewhat rare, but microbial medical scope infections of any kind can be disastrous for patients ill enough to need an ERCP in the first place.
Superbugs like CRE are on the rise independent of the use of medical scopes because of the naturally occurring phenomenon of antibiotic resistance. Bacteria are living things that adapt to the drugs designed to kill them. This leads to dangerous infections for those exposed to superbugs.
It is important to note here that CRE infections do not arise from upper endoscopies or colonoscopies. The particular design of the medical scope used to view the duodenum is responsible for the lingering contamination and does not apply to the scopes used for these other procedures.
Know the Signs of a Medical Scope Infection
Though generally considered safe, there are some side effects to ERCP procedures. After an ERCP procedure, patients can expect mild side effects, such as:
- Bloating and gas for about 24 hours
- A lingering sore throat for a few days
- Slight pain that can be relieved with a heating pad or acetaminophen
More serious side effects could indicate a complication or infection. The signs of a medical scope infection that require prompt medical attention are:
- Severe abdominal pain
- Severe bloating
- Rectal bleeding
- Black stools
- Fever
- Nausea or vomiting
When the infection is caused by CRE bacteria, the symptoms can be diverse and unexpected because the bacteria can travel to any part of the body and cause a seemingly unrelated complication. Some common signs of a CRE infection after an ERCP are:
- Pneumonia
- Shortness of breath
- Urinary tract infection
- Skin infections accompanied by pain and swelling
- Abdominal pain
- Stiff neck and reduced consciousness indicating meningitis
- Fever, chills, and fatigue
At this time, the FDA believes an ERCP is worth the risk of a medical scope infection for any patient ill enough to need one. The agency does not recommend cancelling any scheduled ERCPs. Patients should, however, take note of the symptoms of side effects or complications, and talk to their doctor if they experience signs of an infection.
Medical Device Attorneys offer Legal Guidance
Regardless of the FDA’s continued confidence in the scopes used for ERCPs, people are contracting life-threatening infections, and some people have died due to medical scope infections.
Whether the manufacturer is ultimately responsible, or whether a hospital worker failed to properly process the scope before use, victims should not have to shoulder the financial burden of the illnesses and the life-threatening complications caused by medical scopes. Victims of preventable infections have a right to compensation from the at-fault party.
If you or someone you love has contracted a medical scope infection, Drug and Device Watch attorneys are here to help. Call us today at 1-888-458-6825 to schedule a free consultation, or contact us online.
Sources:
- https://www.cnn.com/2019/04/12/health/medical-scopes-superbug-infections-fda-bn/index.html
- https://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm635828.htm
- https://www.mayoclinic.org/diseases-conditions/infectious-diseases/expert-answers/superbugs/faq-20129283
- https://www.asge.org/home/about-asge/newsroom/transmission-of-cre-bacteria-via-ercp
- https://www.cedars-sinai.org/health-library/diseases-and-conditions/c/carbapenem-resistant-enterobacteriaceae.html